In summary
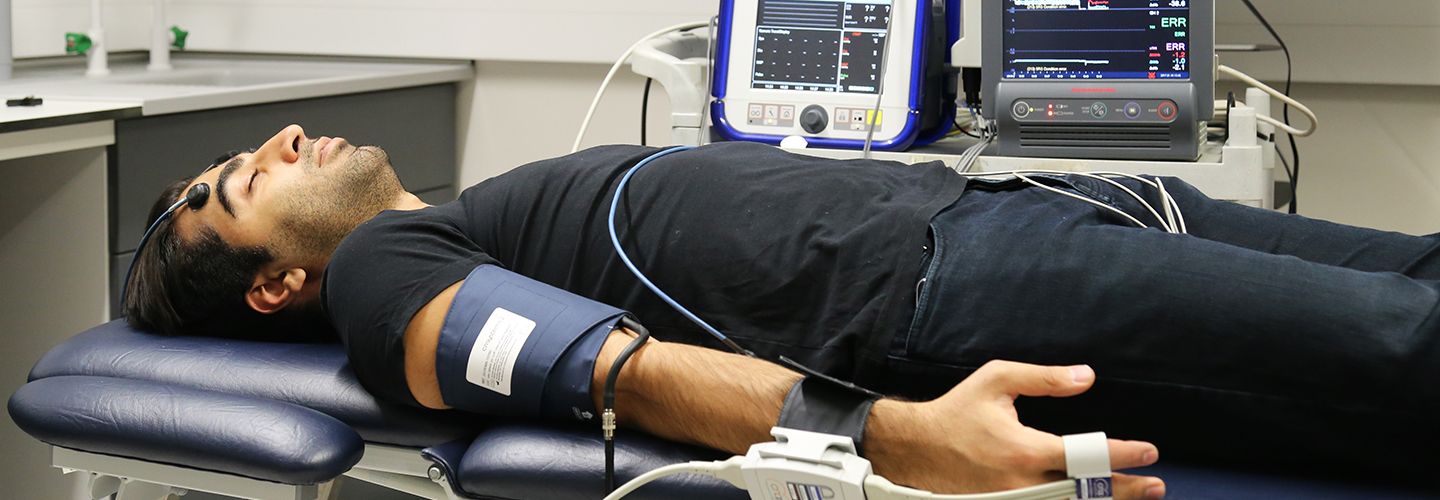
Research undertaken at City, University of London has led to the development of new blood oxygen optical and fibre optic sensors that advance clinical assessment in hospitals by monitoring a patient's arterial blood oxygen in specific organs or tissues.
What did we explore and how?
These sensors are capable of monitoring blood perfusion at times where the current commercial techniques fail to do so and have the advantage of providing organ-specific perfusion (oesophagus, bowel, liver, stomach, brain), enabling the effective monitoring of the wellbeing of specific parts of the body.
These new sensors help clinicians monitor more reliably, in real time, and provide the most appropriate treatment for very sick patients.
Benefits and influence of this research
City researcher Professor P. Kyriacou has involved the design, development and clinical evaluation of a series of optical and fibre optic sensors for monitoring the levels of oxygen and blood volume in arterial and venous blood in critically ill patients (adults, children and neonates).
The basis of this research is the current inability to continuously monitor organ blood oxygen saturation in specific locations (organs and tissues), which prevents the early detection of inadequate tissue oxygenation and so increases the risk of severe lack of oxygen in the blood, multiple organ failure and death.
Current commercial devices require adequate oxygenated blood flow in the extremities to give accurate oxygen saturation results. Poor blood flow is common in decreased blood volume, hypothermia and constriction of the blood vessels, for example, after prolonged operations or in patients suffering with peripheral vascular disease or any other cardiovascular pathologies.
Because conventional pulse oximeters must be attached only to peripheral parts of the body, where pulsating flow is most easily compromised, oxygen readings are unreliable or can cease entirely. Thus, blood oxygen readings may be unavailable at the time when they would be most valuable. Current commercial pulse oximeters will only reveal information about the global perfusion of the body and not specific/regional perfusion.
The application of these new oesophageal, organ and free flap sensors has pushed the boundaries of current practices and clinical monitoring techniques.
Normally, pulse oximeter sensors (used for measuring arterial blood oxygen saturation) are placed on peripheral parts of the body such as the finger, toe or ear lobe. The new sensors can be applied to specific parts of the body such as the oesophagus, bowel, liver, stomach or the 'soft spot' of a newborn baby's skull.
They enable direct monitoring of the viability (wellbeing) of certain organs, tissues or other parts of the body and provide doctors with knowledge of the condition and blood circulation in specific areas which will enhance their assessment, diagnosis and treatment of the patient.